Workers’ Compensation
The Workers’ Compensation program provides statutory benefits for employee injuries arising out of and in the course of employment, and employers’ liability coverage. PERMA uses Athens Administrators for TPA services (see important links and documents in the right hand menu options).
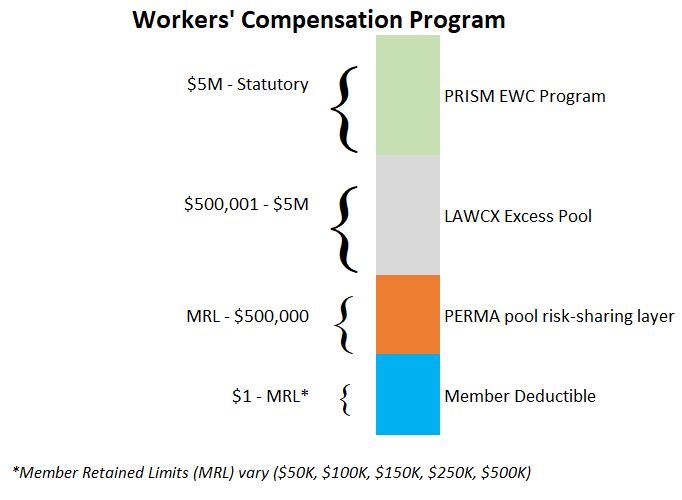
Members may select a self-insured retention of either $50,000, $100,000, $150,000, $200,000, $250,000, or $500,000, pending actuarial review and Executive Committee approval. The pooled coverage limit, per accident, is $500,000 with excess coverage providing statutory limits for workers’ compensation and $5,000,000 for employers’ liability through a combination of pooling and excess coverage. PERMA is a member of the Local Agency Workers’ Compensation Excess Joint Powers Authority (LAWCX) for excess coverage.
LAWCX Risk Control Resources
LAWCX developed a risk control resource webpage so members can more easily access the benefits and services provided under the risk control service plan. Resources include:
- Return-to-Work Program Template
- Wellness Program Tools
- Job Analysis Library and Template
- Infectious Disease Outbreak Response Plan
Benefits of Using Compromise and Release Settlements
Compromise & Release (C&Rs) settlements resolve claims with a final lump sum settlement. The C&R allows employees to gain full control of their medical care, closes the claim (which allows for the elimination of the ongoing administration fees of a claim and unknown and adverse loss development), and allows employees to invest any applicable permanent disability benefits as they receive a lump sum payment versus biweekly payments. In addition to injured workers having more satisfaction regarding medical care control, there is a financial benefit to agencies and pools which utilize C&Rs.
In 2019 LAWCX conducted an actuarial study to learn more about the financial effects of C&Rs on claims. The study grouped claims into permanent disability rating groups (comparing claims of similar seriousness). It compared all claims, large claims ($100k+), cost type (indemnity, medical, expenses), Department (police, fire, non-safety), injury type (sprain/strain, other), and time period (most recent 10 years, older claims). The pool found C&R's saved 25%-47% over stipulated settlements, and 55%-79% more than leaving a claim open.
Additionally, PRISM conducted a study in 2024 to evaluate the difference of resolving WC claims via Compromise & Release (C&R) versus a Stipulated Award. The results included the following:
- C&Rs shortened the life of a claim, when compared to Stipulated awards, by 25% for excess WC members.
- Members with high C&R rates and culture experience a 32% lower loss ratio
PERMA encourages members to speak with their Athens WC adjuster (see listing in the sidebar) to identify claims that may be appropriate for C&R.
Workers’ Compensation Claims Concierge Service
Workers’ Compensation claims are complicated and challenging. Disputes, dissention, litigation, and fraud all tug for claims dollars. PERMA has partnered with ALC Claims Collaboration to offer a claim concierge service that puts the injured worker first and focuses on positive outcomes when there are specific issues, or an employee is uncomfortable with the course of action outlined for the injury. ALC also provides independent review on complex cases to ensure members are comfortable with the case strategy outlined by the adjuster.
To make a referral, the primary workers’ compensation contact at the member agency should email cc@myalcteam.com with the employee’s name, date of injury, and a brief description of the issue at hand, or contact ALC by phone at 949.470.2252. (Spanish bilingual collaborators are available.)
The cost is billed to the claim file as an expense.
Declarations of Workers’ Compensation Coverage
In the past, the “Declarations of Coverage” documents were posted on the PERMA website and emailed to the members.
Beginning with the 2022-23 Program Year, the information has been integrated into the Memorandum of Coverage (MOC) document and thus will no longer be provided separately. Please see pages 2 (Declarations) and 3 (Schedule of Covered Members which includes retentions).
If your agency receives a request from a third party to provide proof of coverage, you can provide the MOC as proof. If the agency will not accept the MOC (e.g. it requested to be named as an “Additional Covered Party” (aka additional insured)), please request a “Certificate of Insurance” from PERMA’s website.